The best time to check in, is now
Most people put off seeing a GP for months. The ones who do best are the ones who didn’t.
1.1 Million Kiwis are uncomfortable talking to their GP about their gut.
It’s time to shatter the taboo and start talking sh*t to save lives
New Zealanders are dying because we find our digestive systems too awkward to discuss
Why your GP needs to hear about your “Command Centre”
Your gut isn’t just a “bathroom issue” — it’s your command centre. A second brain that influences your sleep, mood, energy, and immunity. Your primary defence against chronic disease.
When your gut microbiome is thriving, you feel it — better focus, more stable moods, the kind of energy that doesn’t crash by 3pm. When it’s struggling, you feel that too.
The research is clear: a diverse, well-fed gut microbiome is one of the most powerful levers you have for quality of life. Yet most of us never bring it up with our doctor.
Your GP can’t help with something they don’t know about. So next time you’re in the room — talk about your gut.
Reasons why people don't see their GP
"I'm too embarrassed"
The most common one by far
Your GP has heard it all. Bowel habits, blood, mucus — nothing you say will surprise them. That's literally their job.
"She'll be right"
The Kiwi classic
Statistically, she probably will be. But bowel cancer is the one time she really, really needs to not be.
"I don't have time"
You have time. You just don't want to.
Most GP appointments take less time than scrolling your phone at lunch. Catching something early means far less time dealing with it later.
"I'm scared of what they might find"
The one nobody says out loud
That fear is completely understandable. But not knowing doesn't make it go away. It just gives it more time.
How to stop being weird about it
Reflect on where your awkwardness comes from
Were you raised not to talk about bodies? Did someone shut you down once? Awkwardness usually has a history. Noticing it is the first step to getting past it.
Remind yourself these are just body parts
Anus. Bowel. Stool. They're medical terms for normal parts of a normal body. A GP uses them fifty times a day. The more familiar they become, the less power they have.
Learn from a reputable source
The Gut Foundation has everything you need to understand your gut health. Start here, go deeper. Knowledge makes the conversation easier, with yourself and with your GP.
Book a GP appointment
You don't need a reason. You don't need a serious symptom. You just need to book. Five minutes online, done.
Go to the next page
This one was just for you. The next one is about talking to the people around you. When you're ready.
Before you pop that antibiotic, ask your doctor: do I really need it?
Antibiotics save lives, but only when they’re needed. Aotearoa prescribes more than most developed countries, and a lot of those are for things that would clear up on their own. The problem? Every course wipes out good gut bacteria along with the bad, and your microbiome can take months to recover.
Next time you’re offered a script, just ask: is this one actually necessary?
Antibiotics and your child's gut
The gut microbiome develops most critically in the first three years of life — making early childhood one of the most important windows for gut health. Yet by age five, almost every Kiwi child has had antibiotics — on average, eight courses.
That’s one of the highest rates in the developed world.
Research shows that in the first two years of life, 66% of NZ children received two or more courses, and 31% received five or more. Early antibiotic use disrupts the developing gut microbiome and has been linked to higher rates of asthma, allergies, and obesity — with one study finding obesity prevalence at age five rose steadily with each additional course of antibiotics dispensed.
Read more: Kiwi kids take a lot of antibiotics — here’s why that’s a problem — Newsroom, 2026
There is a lot your gut may be trying to tell you
It’s not just about cancer. Here are the gut conditions your GP can help with.
Most people who go to their GP with gut symptoms don’t have cancer. They have something very treatable — but only if someone knows about it.
IBS — Irritable Bowel Syndrome ▼
One of the most common gut conditions in NZ. Bloating, cramping, diarrhoea and constipation. Very manageable with the right support.
Learn more →Reflux and GORD ▼
Heartburn, acid reflux, a burning feeling in your chest or throat. Extremely common and very treatable.
Learn more →Food intolerances ▼
Lactose, gluten, fructose — many people have intolerances they've been living with for years without knowing.
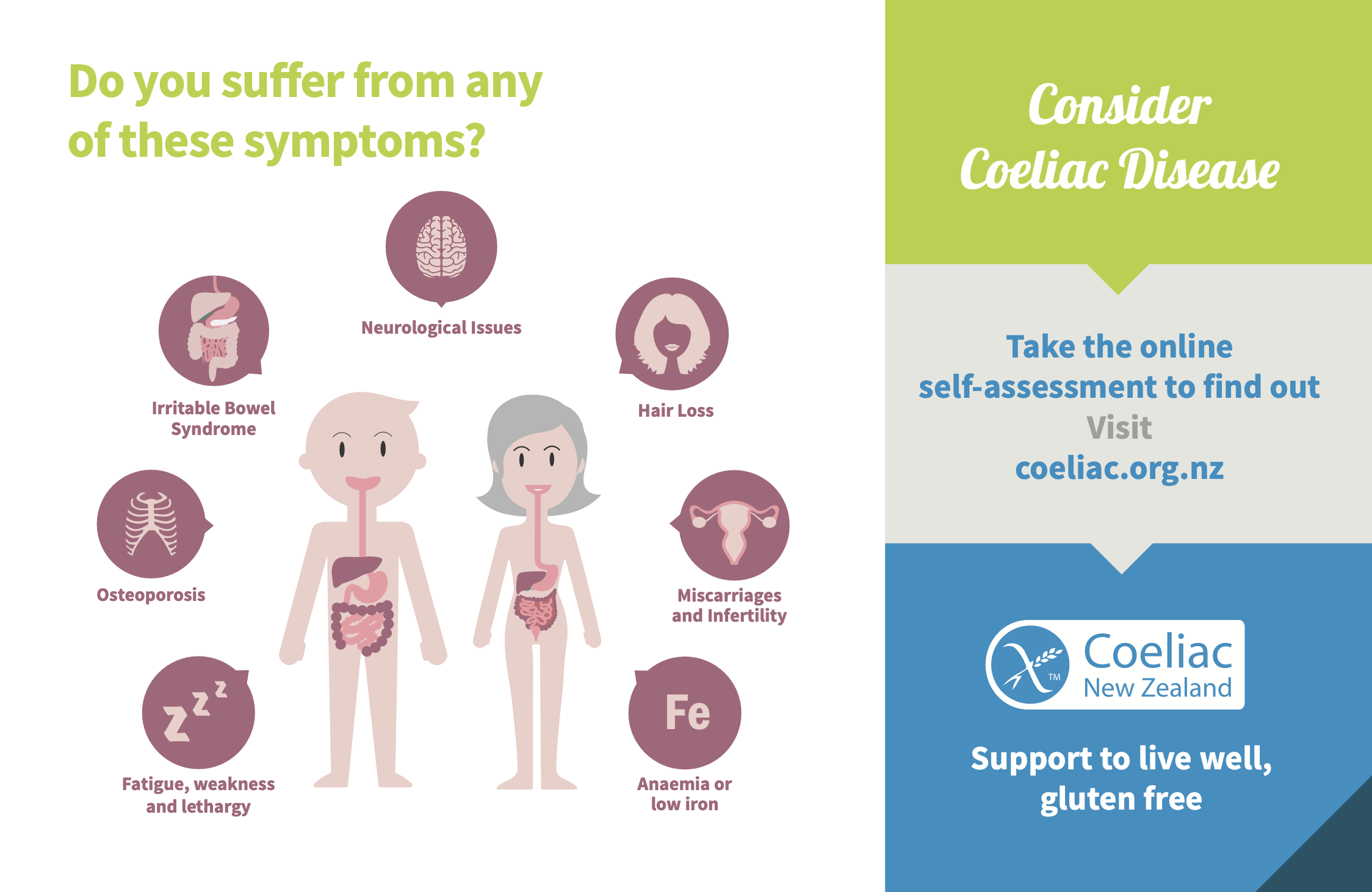
Learn more →Coeliac disease ▼
An autoimmune condition triggered by gluten. Often goes undiagnosed for years. A simple blood test can identify it.
Learn more →SIBO — Small Intestinal Bacterial Overgrowth ▼
Bloating, discomfort, irregular bowel habits caused by a bacteria imbalance. More common than most people realise.
Learn more →IBD — Inflammatory Bowel Disease (Crohn's & Colitis) ▼
Crohn's disease and ulcerative colitis are chronic conditions that cause inflammation in the digestive tract. Symptoms include persistent diarrhoea, abdominal pain, fatigue, and weight loss. New Zealand has one of the highest rates of IBD in the world.
Learn more →Not everything needs a specialist. But everything starts with a conversation with your GP.